Collaboration Blog | Depression Care in Minnesota: We can’t let another year go by.
by: Deb Krause, Vice President for Minnesota Health Action Group; and Liz Cinqueonce, Chief Operating Officer for MN Community Measurement
MN Community Measurement (MNCM) recently released the 2019 Health Care Quality Report. We want to highlight the good news, the troubling news, and the opportunity — with a special focus on mental health and health care in Minnesota.
First, the good news.
- We have a level of transparency about health care quality in Minnesota that other states only aspire to have. The Quality Report is published annually, illuminating trends overall and providing valuable access to quality data at a clinic level. This transparency helps care systems, clinics and health plans understand and improve performance. It also helps individuals (patients and family members seeking care) to make informed choices and seek care from top-performing providers.
- The most recent report highlights one very positive trend for mental health care: Adolescent mental health and/or depression screening has increased from 39.9% of patients in 2015 to 86.1% of patients in 2019. In this time of escalating concern about the mental health of our youth, this is tremendous news. We applaud the clinics that have updated their workflows to improve patient care. Screening to identify those in need of mental health care is an important first step to getting them the care they deserve.
But, the troubling news.
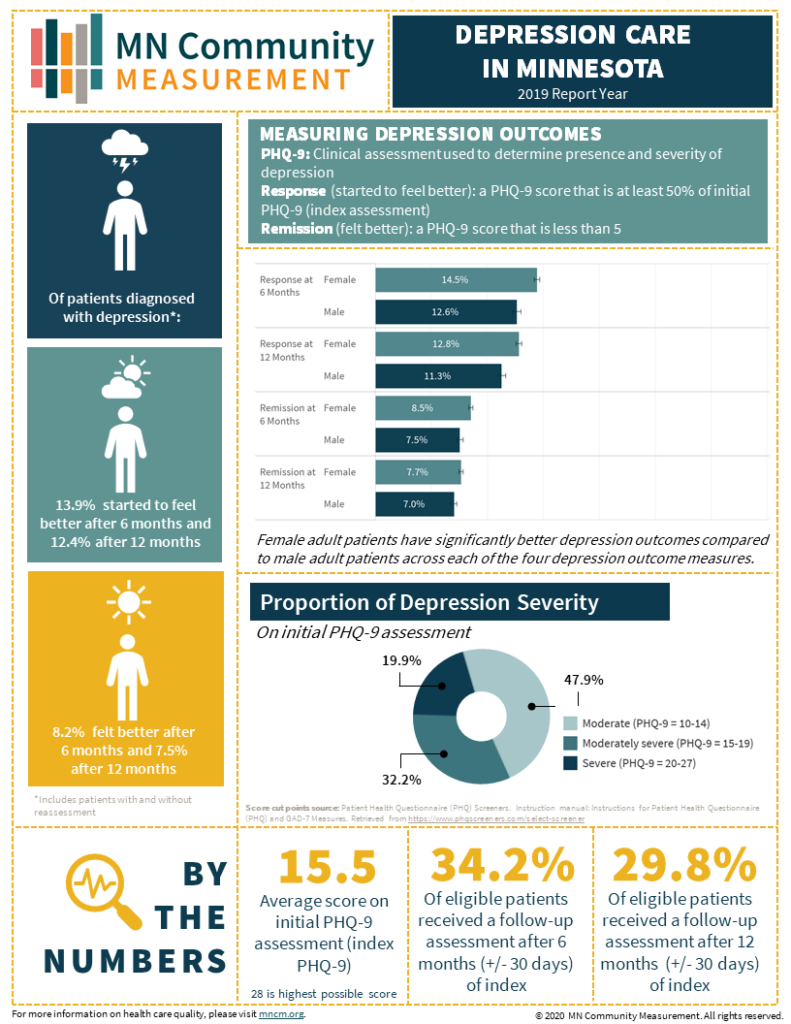
2019 Depression Care
in Minnesota
- Depression remission at 6 months remains “stuck” at a particularly low level — just 8.2% in 2019, compared to 8.0% in 2016. This measures the percentage of patients diagnosed with depression by their primary care providers, who received follow-up and were reassessed at 6 months, and have improved sufficiently to be considered in remission. Mental health conditions are treatable and there are examples of providers in our communities achieving outcomes far above the average. This is what we want for all patients — that they receive good, timely care and get better. But it isn’t happening for most Minnesotans with depression.
- For some other depression measures there was a statistically significant rate increase in the 2019 report, but it falls far short of the outcomes our community expects to achieve. For example, depression remission at 12 months was 7.5% in 2019, up from 6.9% in 2018. Despite the higher rates, the results remain troubling and there is a large opportunity for improvement.
- Finally, there continues to be a considerable gap in performance for mental health outcome measures relative to physical health outcome measures for conditions such as diabetes, cardiovascular or asthma care.
And now, the opportunity.
Given the plateau in depression remission, we offer these words of wisdom from Henry Ford:
“If you always do what you’ve always done, you’ll always get what you’ve always got.”
– Henry Ford
Here are examples of constructive action:
- MNCM’s Board of Directors recently identified improving depression remission as one of its priorities for partnering with others to drive improvement. This will prioritize actions to enhance data reporting, support research to understand barriers, and work with the community to advance solutions.
- The Action Group is conducting important research during 2020 to identify best practices of high-performing clinics with respect to depression remission as part of a prestigious Eugene B. Washington Community Engagement Award from the Patient-Centered Outcomes Research Institute (PCORI). The research will identify best clinical practices and other significant factors associated with clinic performance scores on the depression remission measure. Disseminating the research findings will help providers and their patients in Minnesota and beyond.
- The Path Forward is uniting employers, leading nonprofits, and other stakeholders in Minnesota and across the nation to execute a disciplined, private sector approach to systematically and measurably improve five established best practices of mental health and substance use care.
Measurement is the starting place. Improvement is necessary. Results are the goal.
All stakeholders have a role to play — health plans, care systems and clinics, providers, nonprofits, coalitions, and employers. Let’s hold ourselves accountable for aligning efforts to drive meaningful improvement in depression remission. We can’t let another year go by.
“Without continual growth and progress, such words as improvement, achievement and success have no meaning. “
– Benjamin Franklin
Liz and Deb

Chief Operating Officer
MN Community Measurement

Vice President
Minnesota Health Action Group

